| Indian Academy of Pediatrics Growth Charts Committee, Khadilkar V, Yadav S, Agrawal KK, Tamboli S, Banerjee M, Cherian A, Goyal JP, Khadilkar A, Kumaravel V, Mohan V, Narayanappa D, Ray I, Yewale V (2015) Revised IAP growth charts for height, weight and body mass index for 5- to 18-year-old Indian children. Indian Pediatr 52:47-55. |
Indian Academy of Pediatrics Growth Charts Committee, Khadilkar V, Yadav S, Agrawal KK, Tamboli S, Banerjee M, Cherian A, Goyal JP, Khadilkar A, Kumaravel V, Mohan V, Narayanappa D, Ray I, Yewale V (2015) Indian Pediatr
Abstract: JUSTIFICATION: The need to revise Indian Academy of Pediatrics (IAP) growth charts for 5- to 18-year-old Indian children and adolescents was felt as India is in nutrition transition and previous IAP charts are based on data which are over two decades old.
PROCESS: The Growth Chart Committee was formed by IAP in January 2014 to design revised growth charts. Consultative meeting was held in November 2014 in Mumbai. Studies performed on Indian children's growth, nutritional assessment and anthropometry from upper and middle socioeconomic classes in last decade were identified. Committee contacted 13 study groups; total number of children in the age group of 5 to 18 years were 87022 (54086 boys). Data from fourteen cities (Agartala, Ahmadabad, Chandigarh, Chennai, Delhi, Hyderabad, Kochi, Kolkata, Madurai, Mumbai, Mysore, Pune, Raipur and Surat) in India were collated. Data of children with weight for height Z scores >2 SD were removed from analyses. Data on 33148 children (18170 males, 14978 females) were used to construct growth charts using Cole's LMS method.
OBJECTIVE: To construct revised IAP growth charts for 5-18 year old Indian children based on collated national data from published studies performed on apparently healthy children and adolescents in the last 10 years.
RECOMMENDATIONS: The IAP growth chart committee recommends these revised growth charts for height, weight and body mass index (BMI) for assessment of growth of 5-18 year old Indian children to replace the previous IAP charts; rest of the recommendations for monitoring height and weight remain as per the IAP guidelines published in 2007. To define overweight and obesity in children from 5-18 years of age, adult equivalent of 23 and 27 cut-offs presented in BMI charts may be used. IAP recommends use of WHO standards for growth assessment of children below 5 years of age.
• Bioblast editor: Gnaiger E
| Healthy reference population | Body mass excess | BFE | BME cutoffs | BMI | H | M | VO2max | mitObesity drugs |
From BMI to BME
Work in progress by Gnaiger E 2020-02-10 linked to a preprint in preparation on BME and mitObesity.
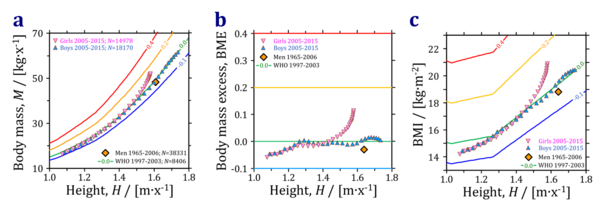
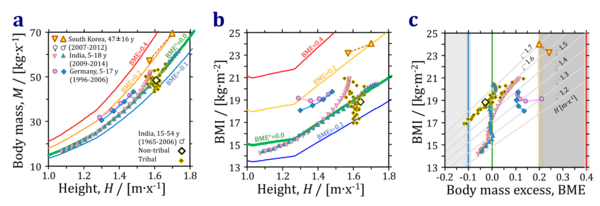
- An increase of the BMI with height is a general feature of the healthy reference population (HRP) with reference body mass, M°, at a body mass excess, BME, of 0.0. The HRP is based on data for WHO Child Growth Standards (WHO Multicentre Growth Reference Study Group, WHO MGRS; WHO 2006 Acta Paediatr; WHO 2006 Geneva: World Health Organization) and the Committee on Biological Handbooks data set (CBH, Zucker 1962 Committee on Biological Handbooks, Fed Amer Soc Exp Biol), compiled from publications between 1931 to 1944 (USA). The average for adult men (India, non-tribal and tribal) and adult women and men from South Korea (Hood 2019 Nutr Diabetes) are shown for comparison (Fig. 1 and 2).
- The 50 centiles were used for height and body mass in each age group. BME and BMI were calculated from the 50 centiles. Calculated (from M and H) and originally published values of the BMI (50 centiles) are idential in girls and boys on average, but the published BMI increases in boys from 20.2 to 21.1 kg·m-2 for height of 1.696 to 1.736 m/x (M 58.2 to 61.6 kg; age 16.5 to 18 years), whereas the calculated BMI increases from 20.2 to 20.4 kg·m-2.
Publications: BME and height
| Reference | |
|---|---|
| Bosy-Westphal 2009 Br J Nutr | Bosy-Westphal A, Plachta-Danielzik S, Dörhöfer RP, Müller MJ (2009) Short stature and obesity: positive association in adults but inverse association in children and adolescents. Br J Nutr 102:453-61. |
| De Onis 2007 Bull World Health Organization | de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J (2007) Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organization 85:660-7. |
| Gnaiger 2019 MiP2019 | OXPHOS capacity in human muscle tissue and body mass excess – the MitoEAGLE mission towards an integrative database (Version 6; 2020-01-12). |
| Hood 2019 Nutr Diabetes | Hood K, Ashcraft J, Watts K, Hong S, Choi W, Heymsfield SB, Gautam RK, Thomas D (2019) Allometric scaling of weight to height and resulting body mass index thresholds in two Asian populations. Nutr Diabetes 9:2. doi: 10.1038/s41387-018-0068-3. |
| Indian Academy of Pediatrics Growth Charts Committee 2015 Indian Pediatr | Indian Academy of Pediatrics Growth Charts Committee, Khadilkar V, Yadav S, Agrawal KK, Tamboli S, Banerjee M, Cherian A, Goyal JP, Khadilkar A, Kumaravel V, Mohan V, Narayanappa D, Ray I, Yewale V (2015) Revised IAP growth charts for height, weight and body mass index for 5- to 18-year-old Indian children. Indian Pediatr 52:47-55. |
| Zucker 1962 Committee on Biological Handbooks, Fed Amer Soc Exp Biol | Zucker TF (1962) Regression of standing and sitting weights on body weight: man. In: Growth including reproduction and morphological development. Altman PL, Dittmer DS, eds: Committee on Biological Handbooks, Fed Amer Soc Exp Biol:336-7. |
MitoPedia: BME and mitObesity
» Body mass excess and mitObesity | BME and mitObesity news | Summary |
| Term | Abbreviation | Description |
|---|---|---|
| BME cutoff points | BME cutoff | Obesity is defined as a disease associated with an excess of body fat with respect to a healthy reference condition. Cutoff points for body mass excess, BME cutoff points, define the critical values for underweight (-0.1 and -0.2), overweight (0.2), and various degrees of obesity (0.4, 0.6, 0.8, and above). BME cutoffs are calibrated by crossover-points of BME with established BMI cutoffs. |
| Body fat excess | BFE | In the healthy reference population (HRP), there is zero body fat excess, BFE, and the fraction of excess body fat in the HRP is expressed - by definition - relative to the reference body mass, M°, at any given height. Importantly, body fat excess, BFE, and body mass excess, BME, are linearly related, which is not the case for the body mass index, BMI. |
| Body mass | m [kg]; M [kg·x-1] | The body mass M is the mass (kilogram [kg]) of an individual (object) [x] and is expressed in units [kg/x]. Whereas the body weight changes as a function of gravitational force (you are weightless at zero gravity; your floating weight in water is different from your weight in air), your mass is independent of gravitational force, and it is the same in air and water. |
| Body mass excess | BME | The body mass excess, BME, is an index of obesity and as such BME is a lifestyle metric. The BME is a measure of the extent to which your actual body mass, M [kg/x], deviates from M° [kg/x], which is the reference body mass [kg] per individual [x] without excess body fat in the healthy reference population, HRP. A balanced BME is BME° = 0.0 with a band width of -0.1 towards underweight and +0.2 towards overweight. The BME is linearly related to the body fat excess. |
| Body mass index | BMI | The body mass index, BMI, is the ratio of body mass to height squared (BMI=M·H-2), recommended by the WHO as a general indicator of underweight (BMI<18.5 kg·m-2), overweight (BMI>25 kg·m-2) and obesity (BMI>30 kg·m-2). Keys et al (1972; see 2014) emphasized that 'the prime criterion must be the relative independence of the index from height'. It is exactly the dependence of the BMI on height - from children to adults, women to men, Caucasians to Asians -, which requires adjustments of BMI-cutoff points. This deficiency is resolved by the body mass excess relative to the healthy reference population. |
| Comorbidity | Comorbidities are common in obesogenic lifestyle-induced early aging. These are preventable, non-communicable diseases with strong associations to obesity. In many studies, cause and effect in the sequence of onset of comorbidities remain elusive. Chronic degenerative diseases are commonly obesity-induced. The search for the link between obesity and the etiology of diverse preventable diseases lead to the hypothesis, that mitochondrial dysfunction is the common mechanism, summarized in the term 'mitObesity'. | |
| Healthy reference population | HRP | A healthy reference population, HRP, establishes the baseline for the relation between body mass and height in healthy people of zero underweight or overweight, providing a reference for evaluation of deviations towards underweight or overweight and obesity. The WHO Child Growth Standards (WHO-CGS) on height and body mass refer to healthy girls and boys from Brazil, Ghana, India, Norway, Oman and the USA. The Committee on Biological Handbooks compiled data on height and body mass of healthy males from infancy to old age (USA), published before emergence of the fast-food and soft-drink epidemic. Four allometric phases are distinguished with distinct allometric exponents. At heights above 1.26 m/x the allometric exponent is 2.9, equal in women and men, and significantly different from the exponent of 2.0 implicated in the body mass index, BMI [kg/m2]. |
| Height of humans | h [m]; H [m·x-1] | The height of humans, h, is given in SI units in meters [m]. Humans are countable objects, and the symbol and unit of the number of objects is N [x]. The average height of N objects is, H = h/N [m/x], where h is the heights of all N objects measured on top of each other. Therefore, the height per human has the unit [m·x-1] (compare body mass [kg·x-1]). Without further identifyer, H is considered as the standing height of a human, measured without shoes, hair ornaments and heavy outer garments. |
| Length | l [m] | Length l is an SI base quantity with SI base unit meter m. Quantities derived from length are area A [m2] and volume V [m3]. Length is an extensive quantity, increasing additively with the number of objects. The term 'height' h is used for length in cases of vertical position (see height of humans). Length of height per object, LUX [m·x-1] is length per unit-entity UX, in contrast to lentgth of a system, which may contain one or many entities, such as the length of a pipeline assembled from a number NX of individual pipes. Length is a quantity linked to direct sensory, practical experience, as reflected in terms related to length: long/short (height: tall/small). Terms such as 'long/short distance' are then used by analogy in the context of the more abstract quantity time (long/short duration). |
| MitObesity drugs | Bioactive mitObesity compounds are drugs and nutraceuticals with more or less reproducible beneficial effects in the treatment of diverse preventable degenerative diseases implicated in comorbidities linked to obesity, characterized by common mechanisms of action targeting mitochondria. | |
| Obesity | Obesity is a disease resulting from excessive accumulation of body fat. In common obesity (non-syndromic obesity) excessive body fat is due to an obesogenic lifestyle with lack of physical exercise ('couch') and caloric surplus of food consumption ('potato'), causing several comorbidities which are characterized as preventable non-communicable diseases. Persistent body fat excess associated with deficits of physical activity induces a weight-lifting effect on increasing muscle mass with decreasing mitochondrial capacity. Body fat excess, therefore, correlates with body mass excess up to a critical stage of obesogenic lifestyle-induced sarcopenia, when loss of muscle mass results in further deterioration of physical performance particularly at older age. | |
| VO2max | VO2max; VO2max/M | Maximum oxygen consumption, VO2max, is and index of cardiorespiratory fitness, measured by spiroergometry on human and animal organisms capable of controlled physical exercise performance on a treadmill or cycle ergometer. VO2max is the maximum respiration of an organism, expressed as the volume of O2 at STPD consumed per unit of time per individual object [mL.min-1.x-1]. If normalized per body mass of the individual object, M [kg.x-1], mass specific maximum oxygen consumption, VO2max/M, is expressed in units [mL.min-1.kg-1]. |
Labels: MiParea: Gender, Exercise physiology;nutrition;life style
Pathology: Aging;senescence, Obesity
Organism: Human
Preparation: Intact organism
BMI, BME, Height

